The Scalpel Free Vasectomy technique or non scalpel vasectomy is the latest non-intrusive technique used to perform a vasectomy.
Vasectomy is the name given to the operation which makes men infertile by producing a block to sperm movement from the testes. A vasectomy and is the most efficient form of permanent male contraception currently available.
In vasectomy the tubes carrying sperm (vas deferens) from the testicles are blocked. This prevents sperm mixing with the semen fluid, making the man sterile.
The production of the male hormone testosterone by the testes is completely unaffected as it all continues to go directly into the bloodstream, hence sex drive and libido are unaltered.
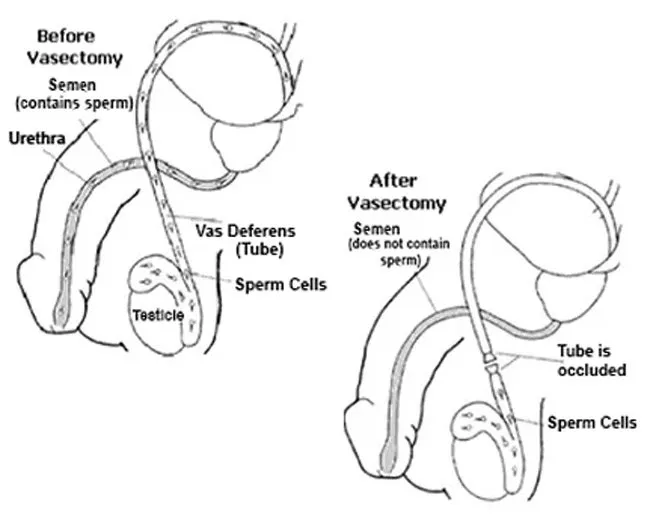

In traditional vasectomy, two incisions (cuts) are made in the scrotum and through these each vas is located, cut and both ends tied.
The skin wounds are closed with stitches. The current recommendation favours minimal invasive techniques such as scalpel free vasectomy (or) no scalpel vasectomy as the preferred method for performing vasectomy.
“Isolation of the vas should be performed using a minimally-invasive vasectomy (MIV) technique such as the no-scalpel vasectomy (NSV) technique or other MIV technique” – American Urological Association
We believe our technical expertise to perform scalpel free vasectomy is the way forward for men to undergo vasectomy.
The Scalpel Free Vasectomy technique (no scalpel vasectomy) has shown to be much superior in reducing postoperative complications such as infections and bleeding rates compared to Scalpel Vasectomy.
Scalpel Free Vasectomy technique (SFV) is a very simple procedure and takes only 10-20 minutes,
perhaps 45 minutes before for discussion including consent and 15 min after operation for recovery. It is performed in our clinic using a special ‘no sting’ local anaesthetic which is injected into the skin in front of the scrotum.
There are no injections into the testes.
Using special instruments, vas tubes are located and isolated from the rest of scrotal structures. With the help of another special equipment that seals the tissue as it cuts, a single small opening, only 2-4mm in size (mini-access) is made in the centre of the scrotum below the penis without using a blade (Scalpel Free Vasectomy technique / no scalpel vasectomy).

This mini access will close rapidly and heal without needing stitches.
A part of the vas tube is removed and ends are sealed without any clips or stitches. Overall, there is very little discomfort and recovery is faster.
Men are not immediately sterile after the operation.
There can be sperm in the ejaculated fluid for many months after the operation (rarely up to 18 months). You must continue to use contraception until postoperative sperm tests have been carried out and you have at least 1 satisfactory sperm test showing no more live (motile) sperm. You will be given further information about this after the operation, before you go home.

10 Reasons Cited by Australian Men When Considering Vasectomy
1. “I (we) don’t want to have (any more) children in the future”
Family Planning: Vasectomy provides a reliable, permanent way to control family size when you’ve decided not to have more children.
2. “We had a scare (Oopsie) and don’t want any Oopsie in the future.”
– Effective Birth Control: It’s one of the most effective forms of contraception available, with a success rate of over 99%, reducing the risk of unintended pregnancies.
3. “I don’t like using condoms.”
– No More Condoms: Say goodbye to the hassle of using condoms and enjoy a more spontaneous and intimate relationship with your partner. However, please remember that condoms protect against sexually transmitted infections, while vasectomy only prevents further pregnancies.
4. “My partner doesn’t want to take the Pill.”
– *No Hormonal Side Effects for Your Partner: However, the decision to have a vasectomy is a man’s decision. There are alternative contraceptive options for women, which you can explore on the full contraceptive options page. If you’ve chosen permanent contraception, vasectomy is the best option to consider.
5. “We can’t afford to have another child.”
– Economic Savings: The cost of raising a child is undoubtedly high. However, your financial situation may change. While financial considerations are common, the decision to have a vasectomy should not be based on finances alone.
6. “It’s easier for me to have the procedure.”
– Quick and Simple Procedure: Yes, vasectomy is a quick and simple procedure, often taking less than 30 minutes, with minimal downtime. It’s a more straightforward option compared to women’s tubal ligation surgery, which requires hospitalization, general anesthesia, longer recovery, and has a higher failure rate in comparison to vasectomy. Additionally, vasectomy is more affordable.
7. “Scalpel-free vasectomy is better than the past methods.”
– Low Complication Rate: Scalpel-Free Vasectomies are considered safe, with a low risk of complications, especially when performed by experienced healthcare providers. They often involve very little or no pain when performed with special combinations of local anesthesia and mini-needle techniques.
8. “She has done her part, and it’s time for me to do mine.”
– Shared Responsibility: Opting for a vasectomy demonstrates shared responsibility for family planning with your partner. Surprisingly, vasectomy appointments have become a unique Valentine’s Day gift!
9. “If we want more children, we’d rather adopt as many children need a good family.”
– Reversibility (in some cases): Although considered permanent, vasectomies can sometimes be reversed through microsurgery if your circumstances change. However, it should primarily be considered a permanent option, as reversibility is not always successful, affordable, or easy to perform. There is no such thing as a “Reversible Vasectomy.”
10. “The world doesn’t need more people.”
– Environmental Impact: Choosing vasectomy as a form of contraception can contribute to reducing the environmental impact associated with population growth. However, this should not be the sole deciding factor for an individual.
In a short line, it is a Man’s individual decision to take control of his contraceptive needs and his future family size.
Vasectomy Reversal
Why do men consider reversal?
\”Approximately 3%–6% of men opt for a vasectomy reversal due to the death of a child or divorce and remarriage, change in financial situation, desire for more children within the same marriage.\” – Patel AP, Smith RP. Vasectomy reversal: a clinical update. Asian J Androl. 2016 May-Jun;18(3):365-71. doi: 10.4103/1008-682X.175091. PMID: 26975488; PMCID: PMC4854082.

Men may consider a reversal of vasectomy for several reasons:
- Desire for More Children: A change in circumstances, such as entering a new relationship or a shift in family planning goals, may lead men to want to have more children after a vasectomy.
- Remarriage or New Partner: If a man remarries or enters a new relationship with a partner who desires children, he may opt for a vasectomy reversal to accommodate their mutual family planning goals.
- Loss of a Child: Tragic events, such as the loss of a child, can profoundly affect a person’s life perspective, leading some men to consider the possibility of expanding their family once again.
- Regret or Change of Heart: Some men may have had a vasectomy when they were younger, and as they age, they may experience a change of heart, feeling regretful about their decision to undergo permanent contraception.
- Emotional and Psychological Factors: The emotional and psychological aspects of fatherhood can be strong motivators. Some men may choose vasectomy reversal to fulfill their emotional and psychological desire to become fathers again.
How Successful are reversals?
Success rates vary from 30% to 95% and depends upon many of the factors as listed below..
Factors that affect the success
1. Time lapsed from vasectomy – longer the time after the vasectomy, the less the success rate.
2. Technique used for reversal – Microsurgical technique and recent advances had improved the success rate.
3. Presence of sperm granuloma – improves the success rate.
4. Age of female partner – not surprisingly younger partner with higher fertility increases success after reversal.
5. Finally the most important factor: Surgeons experience and training in reversal.
Certainly, here’s an expanded explanation of how vasectomy reversal is performed, including the two main procedural techniques:
How is vasectomy reversal done?
Vasectomy reversal is a surgical procedure aimed at restoring a man’s fertility after undergoing a vasectomy. The success of the reversal depends on several factors, including the quality of sperm present in the vasal fluid during the operation.
There are two primary procedural techniques employed for vasectomy reversal, and the choice between them is determined during the surgery based on the surgeon’s assessment of the sperm quality.
- Vasovasostomy: This technique involves reattaching the two cut ends of the vas deferens tube, effectively undoing the vasectomy. The vas deferens is the tube that carries sperm from the testes to the urethra for ejaculation. During a vasovasostomy, the surgeon carefully sutures the severed ends of the vas deferens back together. This procedure is the preferred choice when good-quality sperm are observed in the vasal fluid during surgery. If successful, it allows sperm to once again travel through the vas deferens during ejaculation.
Click here to watch an informative video on Vasovasostomy
Acknowledge source – Mayo Clinic
- Epididymovasostomy: When the surgeon determines that the vasal fluid lacks good-quality sperm or if there is a blockage in the epididymis (the coiled tube where sperm matures and is stored), they may opt for an epididymovasostomy. In this procedure, the cut end of the vas deferens is directly attached to the upper portion of the epididymis. By bypassing the blockage, this technique allows sperm to be transported from the testis to the vas deferens. Epididymovasostomy is a more complex procedure and is typically performed when vasovasostomy is not feasible or successful.
Click here to watch an informative video on Epididymovasostomy
Acknowledge source – Mayo Clinic
The choice between these two techniques is made based on the surgeon’s evaluation of the specific conditions found during the surgery. Both procedures aim to restore the flow of sperm, potentially enabling natural conception. It’s important to note that the success of vasectomy reversal can vary based on various factors, including the length of time since the vasectomy, the surgeon’s experience, and the overall health of the patient.
Where can I get a reversal done?
You should see your GP for a referral to see a urologist who performs vasectomy reversal.
Questions to ask your reversal surgeon?
Experience and Qualifications:
– How many vasectomy reversal procedures have you performed?
– What is your success rate with vasectomy reversals?
– Are you board-certified in urology or a related field?
Assessment and Eligibility:
– Based on my medical history and current health, am I a suitable candidate for vasectomy reversal?
– How long has it been since my vasectomy, and does this impact the chances of success?
Procedure Details
– Can you explain the specific procedure you recommend for me (vasovasostomy or epididymovasostomy)?
– What is the expected duration of the surgery?
– Will it be performed under general or local anesthesia?
Potential Risks and Complications
– What are the potential risks and complications associated with vasectomy reversal?
– How will you address these risks during the procedure?
Recovery and Downtime
– How long is the recovery period after vasectomy reversal?
– Are there any restrictions or lifestyle changes I should be aware of during recovery?
Success and Pregnancy Rates
– What are the chances of a successful reversal in my case?
– Can you provide statistics on pregnancy rates following the procedure?
Cost and Insurance
– What is the estimated cost of the vasectomy reversal procedure?
– Does medicare or Private insurance cover any part of the cost, or do you offer financing options?
Alternative Options
– Are there alternative methods of fertility treatment or family planning if vasectomy reversal is unsuccessful?
Follow-Up Care
– What kind of post-operative care and follow-up appointments will be necessary?
– How will you monitor my progress and fertility after the procedure?
Expectations and Realistic Goals
– What should I realistically expect in terms of recovery time, post-reversal fertility, and potential complications?
– Are there lifestyle changes or habits that can improve the chances of success?
Can I have a vasectomy after Reversal?
– Though vasectomy can be performed after a vasectomy reversal, it is challenging to perform and may require extra measures including use of sedation and some providers may refuse to offer the vasectomy service to patients who have had reversal.
Remember that open and honest communication with your surgeon is crucial to making an informed decision about vasectomy reversal. These questions can serve as a starting point for your discussion, but feel free to ask any additional questions that address your specific concerns and needs.
How much does it cost to have a vasectomy reversal?
The cost of vasectomy reversal varies from provider to provider and you should check with them directly. For a guidance, you should be prepared to pay roughly $10000 or more.
Do you provide vasectomy reversal procedure?
Sorry we don’t. But speak to your GP for your local vasectomy reversal surgeon.
Sperm Banking
Considering Sperm Banking before Your Vasectomy?
You might be wondering about sperm banking as you contemplate a vasectomy. It’s a conversation worth having, especially if you have no children and/or at a young age (<30yrs) when you request for a vasectomy.
Sperm banking is the process of collecting, freezing, and storing sperm for potential future use. It can provide peace of mind but comes at a cost!
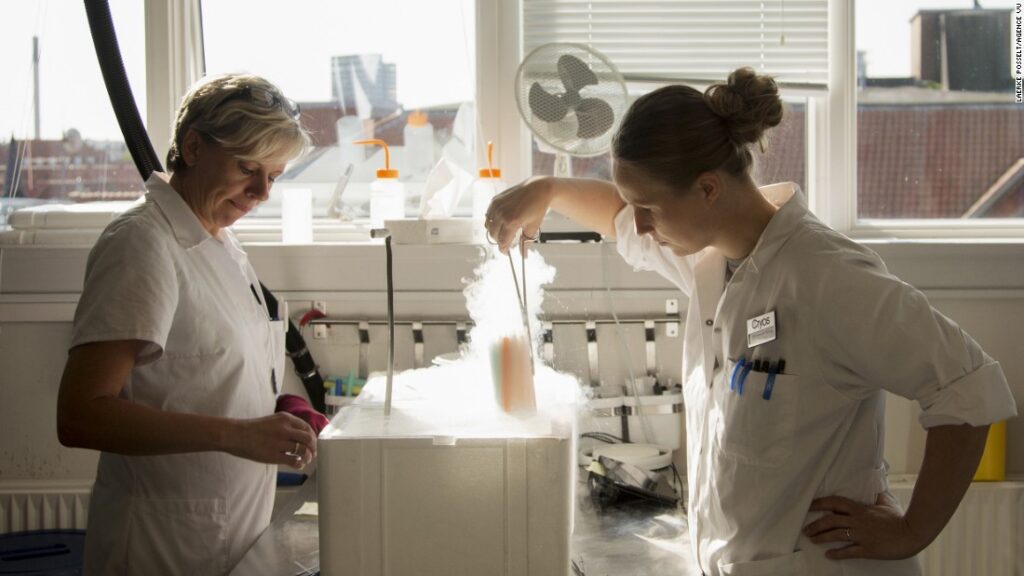
How Does Sperm Banking Work
Here’s a simplified breakdown:
- Screening: You’ll undergo an infectious disease screening to ensure the absence of sexually transmitted diseases for example HIV, Syphilis, Hepatitis B&C.
- Collection: The most common method for sperm collection is masturbation at a fertility clinic.
- Analysis: Andrologists, specialists in sperm and male fertility, analyze your semen sample. They check sperm concentration, morphology (shape), and motility (movement) to ensure it’s healthy and suitable for freezing.
- Freezing: Healthy sperm is placed into a special freezing solution in small vials. These vials go into storage freezers containing liquid nitrogen, maintaining a constant temperature of minus 196 degrees centigrade.
- Thawing: When you’re ready to use the sperm, it’s thawed in the lab until it reaches room temperature. Not all sperm may survive the freeze-thaw process, but those that do may have an advantage in fertility treatments like IVF.
How much does it cost?
The cost varies but generally includes a setup fee (around $500) and annual storage fees ($500 – $800). Please check with the Sperm Banking Service Provider for precise costs.
\”Can I Do It at Home?\” – Silly silly
Unfortunately, successful sperm freezing cannot be done at home due to temperature requirements.
Remember, sperm banking is like insurance for your future. It offers flexibility and peace of mind, especially if you’re considering a vasectomy and haven’t completed your family yet.
Ultimately it depends on if you prepared to pay thousands of dollars over many years for this peace of mind.

Book An Appointment
Simple and Straight forward procedure Walk in, walk out one stop clinic. No Referral Required!
- Simple and Straight Forward Procedure
- Walk-In Walk-Out One Stop Clinic
- Affordable and Effective Permanent Solution
- No GP Referral Required


